Even a single week of restricted sleep can elevate cortisol by 51%, increase hunger hormones by 28%, reduce muscle protein synthesis by 18%, and drop testosterone by 10 to 15%. Here is what the research shows and what you can do about it.
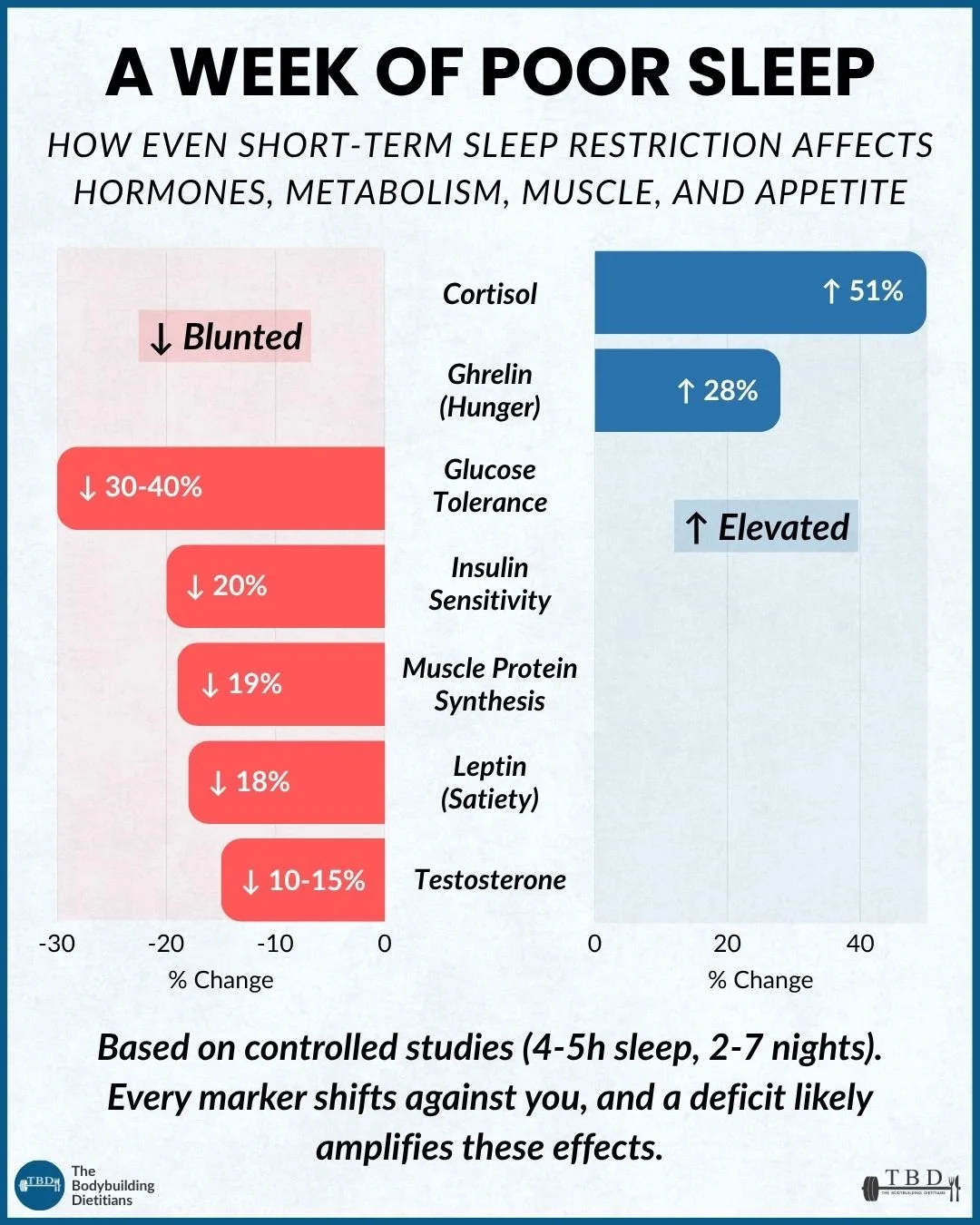
Short-term sleep restriction (four to five hours per night for as few as two to seven nights) produces measurable negative changes across virtually every marker relevant to body composition: cortisol increases by approximately 51%, ghrelin (hunger) rises by 28%, leptin (satiety) falls by 18%, glucose tolerance decreases by 30 to 40%, insulin sensitivity drops by approximately 20%, muscle protein synthesis declines by around 18%, and testosterone falls by 10 to 15%. These effects are amplified during a calorie deficit. Prioritising sleep quality through consistent timing, caffeine management, and a supportive sleep environment is one of the highest-leverage habits available for anyone focused on muscle growth, fat loss, or body composition.
The hormonal and metabolic effects of even short-term sleep restriction are substantial. Every marker relevant to body composition shifts in an unfavourable direction, and a calorie deficit likely amplifies these effects.
Practical, evidence-informed sleep strategies that can be implemented immediately. Consistency in timing and environment tends to have the greatest impact on sleep quality.
The data on what even a week of poor sleep does to your body is fairly hard to ignore. Across a range of well-controlled studies, short-term sleep restriction (typically four to five hours per night for between two and seven consecutive nights) produces unfavourable changes in virtually every hormonal, metabolic, and recovery marker that matters for body composition.
For anyone training consistently and managing their nutrition with the goal of building muscle, losing fat, or improving their physique, sleep is not a peripheral lifestyle factor. It is one of the primary environments in which the body converts training stimulus into actual adaptation. When that environment is compromised, the downstream effects touch everything from how efficiently you use the food you eat, to how much hunger you experience, to how effectively your muscles repair and grow.
The infographic above summarises the key findings from controlled research on short-term sleep restriction. The sections below expand on each one, explain the practical implications for physique-focused individuals, and provide a straightforward set of strategies for improving sleep quality.
How Does Poor Sleep Affect Cortisol and Stress Hormones?
Cortisol, the body's primary stress hormone, increased by approximately 51% in the afternoon and evening period under conditions of sleep restriction, shifting the hormonal environment in a direction that works against both muscle retention and fat loss.
Cortisol is a glucocorticoid hormone produced by the adrenal glands that plays a central role in the stress response, energy mobilisation, and immune regulation. While cortisol serves essential physiological functions (including mobilising energy during training), chronically elevated levels are associated with increased muscle protein breakdown, impaired recovery, reduced insulin sensitivity, and preferential fat storage, particularly in the abdominal region.
In a controlled study, healthy young adults restricted to approximately five hours of sleep per night for one week showed a 51% increase in afternoon and evening cortisol levels compared to baseline, along with significant impairments in glucose metabolism.
Source: Buxton et al., 2010, Diabetes.
The practical implication is straightforward. Elevated cortisol shifts the hormonal environment toward catabolism (tissue breakdown) rather than anabolism (tissue building). For someone training to build or retain muscle, this means the recovery process is being run against a headwind. The training stimulus may be excellent, the nutrition may be well-structured, but if the hormonal environment in which recovery occurs is compromised by insufficient sleep, the return on that investment is diminished.
This effect becomes especially relevant during a calorie deficit, where cortisol levels are already elevated as a normal response to energy restriction. Layering poor sleep on top of a deficit creates a compounding effect that accelerates many of the negative adaptations associated with extended dieting: increased hunger, reduced energy, impaired recovery, and a hormonal profile that is less favourable for preserving lean mass.
How Does Sleep Restriction Affect Hunger and Appetite?
Sleep restriction increases ghrelin (the primary hunger hormone) by approximately 28% while reducing leptin (the primary satiety hormone) by approximately 18%, creating a hormonal environment that drives increased food intake and a specific pull toward calorie-dense, carbohydrate-rich foods.
Ghrelin is a peptide hormone produced primarily in the stomach that stimulates appetite and food intake. Ghrelin levels typically rise before meals and fall after eating. Leptin is a hormone produced by fat cells that signals energy status to the brain and promotes satiety. When leptin levels are reduced, the brain interprets this as a signal of energy insufficiency, which increases hunger and drives food-seeking behaviour.
A landmark study on sleep and appetite hormones found that two nights of sleep restriction (four hours per night) increased ghrelin by 28%, decreased leptin by 18%, and was associated with a 24% increase in self-reported hunger ratings, with a specific shift in food preference toward calorie-dense, carbohydrate-rich options.
Source: Spiegel et al., 2004, Annals of Internal Medicine.
If you have ever noticed that food feels harder to control after a rough week of sleep, that is not a lack of discipline. It is a measurable, physiologically driven shift in appetite hormones that makes hunger more intense and satiety signals weaker. For someone in a calorie deficit, where hunger management is already one of the most challenging aspects of the process, this hormonal shift can make the difference between a manageable phase and one that feels unsustainable.
In coaching settings, a common pattern is for athletes to report increased cravings, food focus, and difficulty adhering to their nutrition plan during periods of poor sleep, without recognising that the sleep itself is the primary driver. Addressing the sleep deficit often resolves these symptoms more effectively than adjusting the diet, which is a useful insight for anyone who finds their dietary adherence deteriorating for no obvious nutritional reason.
What Happens to Glucose Tolerance and Insulin Sensitivity?
Glucose tolerance decreases by 30 to 40% and insulin sensitivity drops by approximately 20% under conditions of short-term sleep restriction, meaning the body handles carbohydrates significantly less efficiently.
Glucose tolerance refers to the body's ability to clear glucose from the bloodstream efficiently after a meal. Insulin sensitivity refers to how effectively the body's cells respond to insulin, the hormone responsible for facilitating glucose uptake. When insulin sensitivity is reduced, higher levels of insulin are required to achieve the same effect, which can promote fat storage and impair the body's ability to use carbohydrate as fuel.
In one of the earliest and most frequently cited studies on sleep and metabolism, healthy young adults restricted to four hours of sleep per night for six consecutive nights showed glucose tolerance levels and insulin sensitivity profiles that resembled those of individuals in the early stages of type 2 diabetes, despite having no metabolic conditions at baseline.
Source: Spiegel et al., 1999, The Lancet.
For physique-focused individuals, reduced insulin sensitivity has practical consequences beyond the metabolic health implications. Carbohydrate is the primary fuel for high-intensity resistance training, and the body's ability to store and utilise glycogen depends in part on insulin sensitivity. When sensitivity is reduced, carbohydrate handling becomes less efficient, which can affect training performance, recovery, and the body's ability to direct nutrients toward muscle rather than fat storage.
This does not mean that carbohydrate intake should be reduced in response to poor sleep. The more productive response is to address the sleep itself, because the impairment in glucose metabolism is a consequence of the sleep restriction rather than a permanent metabolic state. Improving sleep quality typically restores glucose tolerance and insulin sensitivity within days, which is a far more effective intervention than manipulating macronutrient intake to compensate.
How Does Sleep Affect Muscle Protein Synthesis and Recovery?
Muscle protein synthesis, the process through which training stimulus is converted into actual muscle repair and growth, decreases by approximately 18% under conditions of sleep restriction, alongside an increase in catabolic markers.
Muscle protein synthesis (MPS) is the biological process through which dietary protein and the mechanical stimulus from resistance training combine to drive the repair and growth of skeletal muscle tissue. MPS is the primary mechanism through which training leads to muscle adaptation, and it is highly sensitive to the availability of amino acids, the quality of the training stimulus, and the recovery environment in which it occurs.
A study examining the effects of sleep restriction on skeletal muscle protein metabolism found that five nights of restricted sleep (approximately five hours per night) reduced muscle protein synthesis rates by approximately 18% and increased markers of muscle protein breakdown compared to a normal sleep condition in healthy young adults.
Source: Lamon et al., 2021, Physiological Reports.
This finding is perhaps the most directly relevant for anyone training consistently. The work done in the gym applies the stimulus. Sleep is a critical part of the environment in which the body converts that stimulus into actual structural adaptation. When sleep is compromised, the efficiency of that conversion process is reduced, which means that the same training session produces less adaptation than it would under adequate sleep conditions.
Over a single poor night, this effect is unlikely to be meaningful. Over weeks and months of chronically insufficient sleep, however, the cumulative effect on muscle accrual and recovery is substantial. For athletes in an improvement season, where the entire goal is to maximise the muscle-building response to training, chronic sleep restriction represents a significant and entirely avoidable limitation on progress. For athletes in a deficit, where muscle protein synthesis rates are already suppressed by the energy restriction itself, the compounding effect of poor sleep on MPS makes lean mass preservation considerably more difficult.
What Happens to Testosterone When You Don't Sleep Enough?
Testosterone levels decline by 10 to 15% after just one week of sleeping five hours per night, a reduction equivalent to approximately ten to fifteen years of normal age-related decline compressed into seven days.
Testosterone is an anabolic steroid hormone that plays a central role in muscle protein synthesis, recovery, bone density, mood, and overall physiological function in both men and women. While testosterone is often discussed primarily in the context of male physiology, it is relevant for female athletes as well, as it contributes to muscle growth, strength, and recovery capacity at the concentrations present in women.
A study in healthy young men found that one week of sleep restriction to five hours per night resulted in a 10 to 15% decrease in daytime testosterone levels. For context, normal age-related testosterone decline runs at approximately 1 to 2% per year from the age of 30 onwards, meaning that a single week of restricted sleep compressed roughly a decade of age-related decline into seven days.
Source: Leproult and Van Cauter, 2011, JAMA.
The practical relevance for physique-focused individuals is clear. Testosterone is one of the most important hormonal drivers of muscle growth and recovery. While the reductions observed in sleep restriction studies are acute and reversible (testosterone levels recover when sleep is restored), chronic sleep restriction maintains this suppression indefinitely, creating a persistently less favourable hormonal environment for training adaptation.
For natural athletes in particular, where the hormonal ceiling for anabolic signalling is already lower than in enhanced counterparts, any further suppression of testosterone from inadequate sleep represents a meaningful reduction in their capacity for muscle growth. This makes sleep one of the few genuinely controllable variables that directly influences the hormonal environment in which training adaptations occur.
Why Does Sleep Matter Even More During a Calorie Deficit?
Every negative effect of sleep restriction is amplified during a calorie deficit, because the physiological stress of energy restriction compounds with the physiological stress of insufficient sleep.
During a deficit, cortisol is already elevated, leptin is already reduced, ghrelin is already increased, and muscle protein synthesis rates are already lower than during maintenance or surplus conditions. These are normal, expected adaptations to energy restriction. Layering poor sleep on top of these existing adaptations creates a compounding effect that accelerates the decline in every relevant marker.
A study comparing the effects of sleep duration on body composition during a calorie deficit found that participants who slept 8.5 hours per night lost a similar amount of total weight to those who slept 5.5 hours, but the sleep-restricted group lost significantly more lean mass and less fat mass. The well-rested group preserved muscle more effectively and lost a greater proportion of their weight as body fat.
Source: Nedeltcheva et al., 2010, Annals of Internal Medicine.
This study is one of the most directly relevant pieces of evidence for anyone managing a fat loss phase. The total weight loss was comparable between groups, but the composition of what was lost changed dramatically based on sleep. The practical implication is that two people following the same diet and training plan can achieve very different body composition outcomes based on sleep alone, with the sleep-deprived individual losing more muscle and less fat.
For competitors in contest preparation, where the entire goal is to maximise fat loss while preserving as much lean mass as possible, this finding positions sleep as one of the most impactful variables in the process. Optimising nutrition, training, and supplementation while neglecting sleep is a strategy with a fundamental blind spot.
What Can You Do to Improve Sleep Quality?
The practical side of improving sleep quality is not complicated. A small number of evidence-informed habits, applied consistently, can produce meaningful improvements in both sleep duration and sleep quality.
Consistent bed and wake times. Maintaining a regular sleep schedule, even on weekends, is probably the single highest-leverage sleep habit available. The body's circadian rhythm is calibrated by consistency, and irregular sleep timing disrupts the hormonal signals (melatonin, cortisol) that regulate sleep onset and wakefulness. Aiming to keep bed and wake times within a 30-minute window across the week provides a strong foundation for sleep quality.
Circadian rhythm refers to the approximately 24-hour internal clock that regulates the sleep-wake cycle, hormone release, body temperature, and other physiological processes. It is primarily entrained by light exposure and meal timing, and it functions most effectively when daily routines are consistent.
Caffeine management. Caffeine has a half-life of approximately five to six hours, meaning that half of the caffeine consumed is still active in the body five to six hours later. A pre-workout supplement or energy drink consumed at 3:00 pm still has meaningful stimulant effects at 9:00 pm. Stopping caffeine by early afternoon (at least six to eight hours before the intended bedtime) is one of the most effective interventions for improving sleep onset and depth. This includes pre-workout supplements and energy drinks, which people often overlook when thinking about their caffeine intake.
Light environment. Getting direct sunlight exposure early in the day helps anchor the circadian rhythm and supports natural melatonin production in the evening. In the hours before bed, reducing exposure to bright overhead lighting and blue-light-emitting screens supports the transition toward sleep. Moving the phone to a different room before bed eliminates the temptation to scroll and removes one of the most common sources of pre-sleep stimulation.
Melatonin is a hormone produced by the pineal gland that signals the onset of darkness to the body and promotes sleep. Melatonin production is suppressed by light exposure, particularly blue-spectrum light from screens, and is enhanced by darkness and consistent sleep timing.
Room temperature. A bedroom temperature of approximately 18 to 20 degrees Celsius supports the natural drop in core body temperature that occurs during sleep onset. Blackout curtains or a sleep mask can further improve the light environment, particularly for people who train early in the morning and need to sleep while it is still light outside.
Pre-sleep routine. Establishing a consistent wind-down routine of 20 to 30 minutes before bed gives the nervous system a chance to transition from a state of alertness to a state conducive to sleep. This does not need to be elaborate. Dimming lights, light stretching, reading, or simply sitting quietly can be enough. The consistency of the routine matters more than the specific activities.
Meal timing. Large meals within approximately two hours of sleep can disrupt sleep quality by increasing core body temperature and demanding active digestion during a period when the body should be transitioning into rest. This does not mean you need to avoid eating in the evening, but spacing the largest meal of the day at least two hours before bed tends to support better sleep quality without requiring a dramatic change to the overall meal schedule.
Alcohol. Alcohol is commonly perceived as a sleep aid because it can reduce sleep onset latency (the time it takes to fall asleep). However, alcohol significantly reduces REM sleep quality, increases sleep fragmentation in the second half of the night, and suppresses growth hormone release during sleep. Even moderate alcohol consumption close to bedtime has a measurable negative effect on sleep architecture and recovery.
If you are managing a calorie deficit or preparing for a competition and want to ensure that your sleep habits are supporting your broader nutrition and training goals, a consultation with one of our dietitians can help you identify where practical adjustments to your routine can make the most difference.
Practical Takeaways
Even short-term sleep restriction (four to five hours per night for as few as two to seven nights) produces measurable negative changes across every hormonal and metabolic marker relevant to body composition, including cortisol, ghrelin, leptin, glucose tolerance, insulin sensitivity, muscle protein synthesis, and testosterone.
These effects are amplified during a calorie deficit, where the physiological stress of energy restriction compounds with the physiological stress of poor sleep. Research shows that sleep-restricted individuals in a deficit lose more lean mass and less fat mass than well-rested individuals on the same diet.
A consistent bed and wake time, even on weekends, is likely the single highest-leverage sleep habit. Keeping this within a 30-minute window across the week provides a strong circadian foundation.
Stop caffeine by early afternoon (at least six to eight hours before bed), including pre-workout supplements and energy drinks that are often overlooked as caffeine sources.
Optimise the sleep environment: cool room (18 to 20 degrees Celsius), blackout curtains or sleep mask, phone in a different room, and reduced screen and overhead lighting in the hour before bed.
Sleep is not a peripheral lifestyle factor for physique-focused individuals. It is one of the primary environments in which training stimulus is converted into actual adaptation, and neglecting it creates a blind spot that no amount of nutritional or training optimisation can fully compensate for.
Frequently Asked Questions
How many hours of sleep do you need to build muscle?
Most research on sleep and recovery supports a target of seven to nine hours per night for physically active individuals. The studies showing significant impairment in muscle protein synthesis, testosterone, and recovery markers typically used restriction protocols of four to five hours per night, suggesting that consistently sleeping below six hours carries meaningful risk for muscle-building outcomes. Individual needs vary, but aiming for at least seven hours of quality sleep provides a reasonable foundation.
Does poor sleep cause muscle loss?
Poor sleep does not directly cause muscle loss in the way that prolonged inactivity or severe energy restriction can, but it reduces the rate of muscle protein synthesis by approximately 18% and creates a hormonal environment (elevated cortisol, reduced testosterone) that is less favourable for muscle retention. During a calorie deficit, sleep-restricted individuals have been shown to lose significantly more lean mass than well-rested individuals following the same diet, indicating that sleep plays a meaningful role in preserving muscle during fat loss.
Can lack of sleep make you gain fat?
Sleep restriction does not directly cause fat gain, but it creates conditions that make fat gain more likely. Increased ghrelin and decreased leptin drive greater hunger and a preference for calorie-dense foods, while reduced insulin sensitivity impairs the body's ability to handle carbohydrate efficiently. During a calorie deficit, research shows that sleep-restricted individuals lose proportionally less fat and more lean mass compared to those sleeping adequately. Over time, these effects can meaningfully influence body composition even when calorie intake is controlled.
Does caffeine before a workout affect sleep?
Caffeine has a half-life of approximately five to six hours, meaning that a significant proportion of the caffeine from a pre-workout supplement consumed in the mid-to-late afternoon is still active at bedtime. This can delay sleep onset, reduce sleep depth, and impair sleep quality even if the individual feels they can fall asleep without difficulty. Stopping all caffeine sources by early afternoon (at least six to eight hours before the intended bedtime) is one of the most effective interventions for protecting sleep quality.
Does alcohol affect sleep quality?
Alcohol reduces REM sleep quality, increases sleep fragmentation (particularly in the second half of the night), and suppresses growth hormone release during sleep. While alcohol can reduce the time it takes to fall asleep, the overall effect on sleep architecture and recovery is negative. Even moderate alcohol consumption close to bedtime has been shown to impair recovery-related sleep processes, making it a meaningful consideration for anyone prioritising training adaptation and body composition.
How quickly do the effects of poor sleep reverse?
Most of the acute hormonal and metabolic effects of short-term sleep restriction (elevated cortisol, impaired glucose tolerance, reduced testosterone) begin to reverse within a few days of returning to adequate sleep. However, the body composition consequences of chronic sleep restriction (preferential lean mass loss during a deficit, reduced cumulative muscle protein synthesis) cannot be retroactively corrected. The lost adaptation opportunity during the period of poor sleep is lost. This makes consistent sleep quality a priority throughout training and dieting phases rather than something to address only after problems have emerged.
If you would like support building a nutrition and lifestyle plan that accounts for sleep, recovery, and the broader factors that influence body composition, our team of qualified dietitians can help.