Diet fatigue is a normal and predictable feature of sustained energy restriction. Understanding the physiological and psychological mechanisms behind it, how to recognise when it requires action, and the strategies that help extend productive dieting changes how effectively a fat loss phase can be managed.
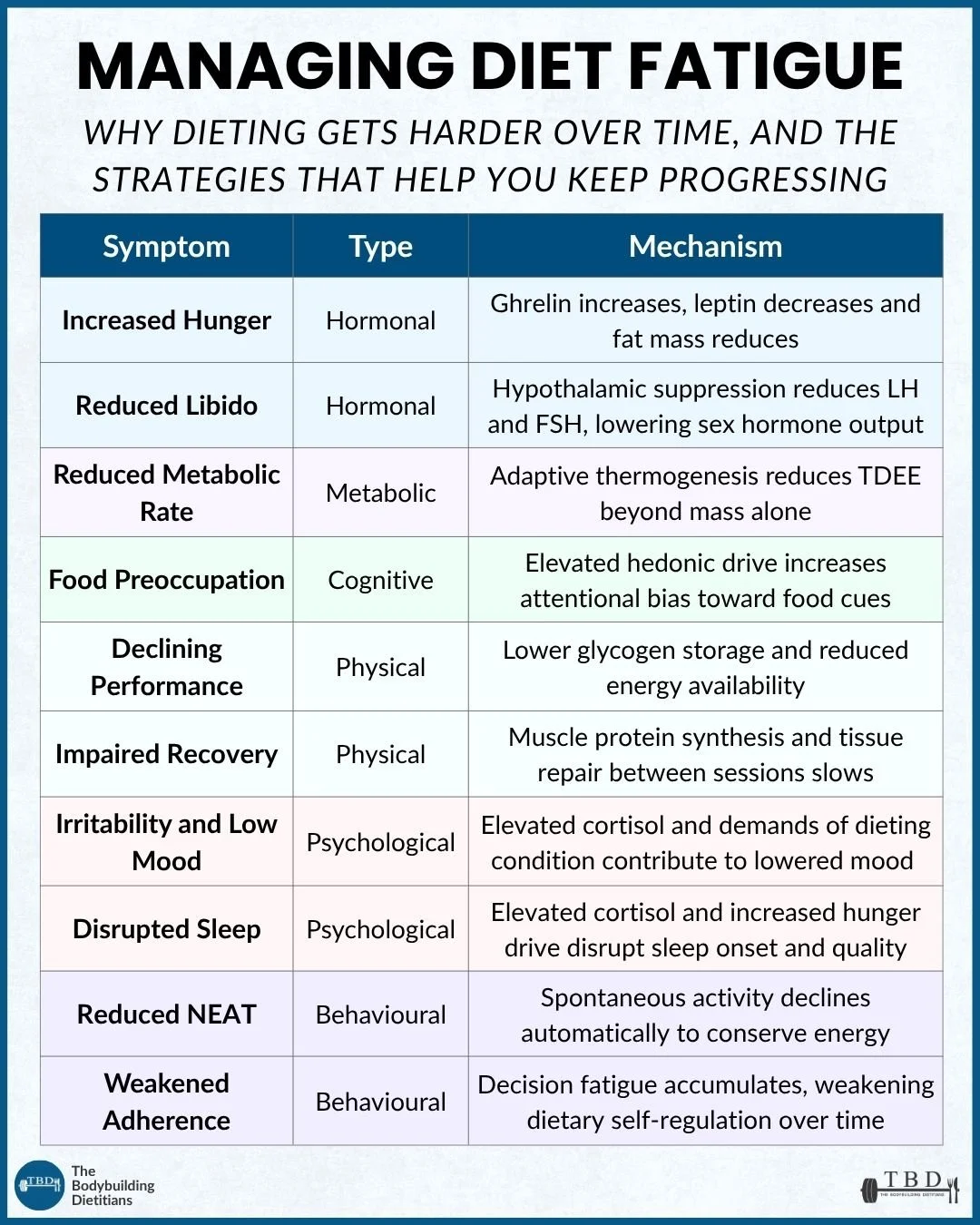
Diet fatigue refers to the accumulation of physiological and psychological symptoms that develop during sustained energy restriction. The mechanisms are well-characterised: ghrelin rises and leptin falls as fat mass decreases, increasing hunger and reducing satiety; adaptive thermogenesis reduces total daily energy expenditure beyond mass loss alone; NEAT declines automatically; sleep is disrupted; mood and stress tolerance worsen; and dietary adherence becomes progressively harder as decision fatigue accumulates. These are adaptive responses to prolonged calorie deficit, not signs of inadequate motivation. Management strategies include calibrating expectations appropriately, implementing structured diet breaks of one to two weeks at maintenance calories, and using refeeds around training. Knowing when to end a fat loss phase entirely, rather than continuing into diminishing returns, is equally important.
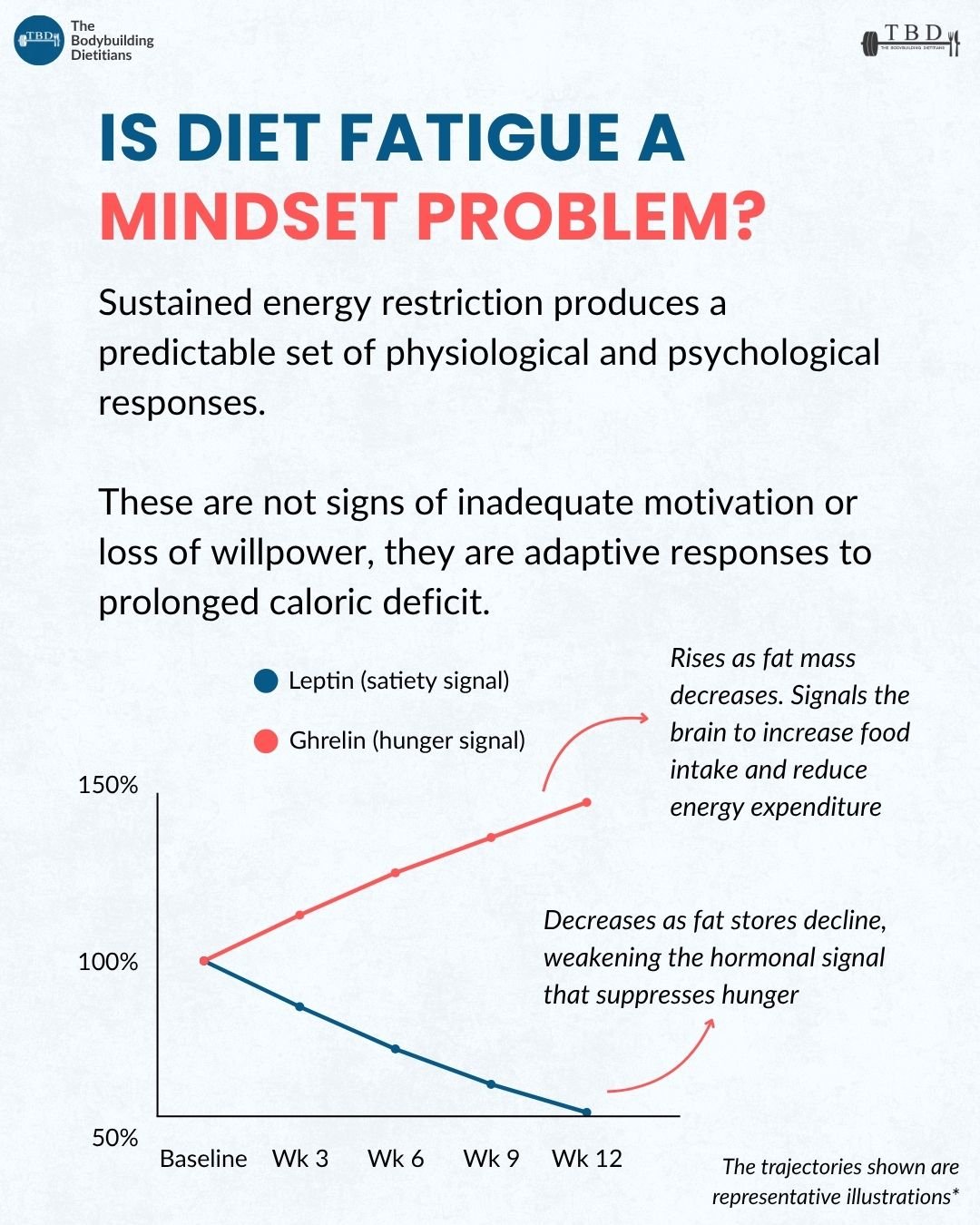



Diet fatigue is not a sign that a diet is failing. It is one of the more reliably predictable features of sustained energy restriction, and the physiological and psychological mechanisms that drive it are well-characterised in the research. Ghrelin rises, leptin falls, NEAT declines, mood worsens, sleep becomes disrupted, and adherence becomes progressively more effortful. These are not consequences of insufficient willpower or inadequate motivation. They are adaptive responses the body uses to defend against a prolonged calorie deficit, and they appear across virtually every individual who sustains meaningful energy restriction over time.
Understanding this does not make the experience less difficult. But it does change how rationally someone can respond to it, and that response is where the practical management of a fat loss phase either succeeds or falls apart.
What Is Diet Fatigue and Why Does It Happen?
Diet fatigue is the accumulation of physiological and psychological symptoms that develop as a fat loss phase extends in duration. It is not a single symptom but a cluster of overlapping responses across hormonal, metabolic, cognitive, physical, psychological, and behavioural domains, each with a distinct mechanism and each compounding the others.
The hormonal component is perhaps the most fundamental. Leptin is a hormone produced by adipose tissue that signals satiety to the brain. As fat mass decreases during a diet, leptin production falls, weakening the hormonal signal that suppresses hunger and supports energy expenditure. Ghrelin, the primary hunger-stimulating hormone, rises in response to calorie restriction and reduced fat mass, signalling the brain to increase food intake and reduce energy expenditure. The combined effect is that hunger becomes more intense and the experience of fullness becomes less reliable over the course of a diet, not because the person is losing discipline, but because the hormonal environment has shifted in a direction that opposes continued restriction.
Leptin and ghrelin are both influenced by fat mass, energy intake, and the duration of restriction. The trajectories shown in the carousel are representative: across a twelve-week fat loss phase, leptin can decline significantly while ghrelin rises, producing an increasingly demanding hormonal context that makes dietary adherence harder as the diet progresses even as total calorie intake may not change.
The metabolic component adds another layer. Adaptive thermogenesis refers to the reduction in total daily energy expenditure that occurs during sustained calorie restriction beyond what would be predicted from mass loss alone. As the body recognises the deficit, it reduces metabolic rate through reductions in thyroid hormone activity, sympathetic nervous system output, and non-resting energy expenditure. The practical effect is that a given calorie intake produces less fat loss over time than it did at the start of the diet, not because the individual is doing anything differently, but because the body has partially compensated.
The behavioural component includes NEAT reduction, which is one of the most underappreciated mechanisms of adaptive thermogenesis. NEAT, or non-exercise activity thermogenesis, refers to all movement outside of structured exercise, including walking, fidgeting, and incidental daily activity. As a diet extends, spontaneous physical activity tends to decline automatically, often without the individual being consciously aware of it. This reduction can account for a meaningful portion of the metabolic adaptation observed in prolonged dieters and is one reason that maintaining step count deliberately becomes more important, not less, as a fat loss phase progresses.
A controlled study by Leibel et al. found that a 10 percent reduction in bodyweight was associated with an average decrease in total daily energy expenditure of approximately 15 percent in obese participants and 22 percent in those who had never been obese, reflecting the contribution of adaptive thermogenesis beyond the reduction expected from mass loss alone.
Source: Leibel et al., 1995, New England Journal of Medicine.
What Are the Signs That Diet Fatigue Is Setting In?
Recognising diet fatigue requires monitoring a broader set of signals than scale weight alone. Because the symptoms span multiple domains and develop gradually, they can be easy to attribute to other causes or to dismiss as temporary if they are assessed in isolation. A cluster of signals appearing around the same period is more meaningful than any single symptom.
Adherence declining despite consistent effort is one of the earlier and more reliable signals. This is distinct from poor planning or inconsistent tracking: the individual is engaging with the diet actively, but maintaining restraint is requiring noticeably more cognitive effort than it did earlier in the phase. This reflects the combination of rising hunger drive, elevated hedonic sensitivity to food cues, and the accumulation of decision fatigue across weeks of continuous dietary regulation.
Persistent food preoccupation, particularly in the evening, is another recognisable pattern. The elevated hedonic drive that develops during calorie restriction increases attentional bias toward food-related stimuli, which is the brain responding to an energy deficit by prioritising food-seeking behaviour. Thinking about food more frequently between meals, particularly at times when hunger is highest and cognitive resources are lowest, is a normal feature of advanced diet fatigue rather than a psychological weakness.
Declining training performance or motivation is a physical signal with a clear mechanism: lower glycogen availability, reduced energy availability, and slower recovery between sessions all reflect the physiological cost of the deficit accumulating. Training performance tends to decline before visible changes in muscle mass, making it a useful early warning signal that the deficit is affecting the body's capacity to sustain productive training.
Irritability, reduced stress tolerance, and disrupted sleep are the psychological signals. Elevated cortisol from prolonged energy restriction contributes to mood changes and reduced tolerance for stressors that would otherwise be manageable. Disrupted sleep onset and sleep quality reflect the combined effect of elevated cortisol and the difficulty of falling asleep with a hungry stomach, both of which are direct consequences of the dieting state.
A sense of fatigue disproportionate to training load, and genuinely not enjoying the process anymore, are late-stage signals that warrant a meaningful adjustment rather than minor tweaks. One signal appearing in isolation is not necessarily cause for intervention. Multiple signals clustering together, particularly across hormonal, physical, and psychological domains simultaneously, is a reliable indicator that the diet requires some form of modification.
What Strategies Help Manage Diet Fatigue?
Three broad categories of strategy address diet fatigue effectively: expectations management, diet breaks, and refeeds. Each operates through a different mechanism and is appropriate in different circumstances.
Expectations management The most consistent and underappreciated determinant of how well someone tolerates a difficult fat loss phase is whether they understood in advance that difficulty was coming. Individuals who enter a diet expecting it to feel progressively harder, and who understand the physiological reasons why, are considerably better placed to respond to that difficulty with problem-solving rather than self-criticism.
Reframing diet fatigue as a physiological process rather than a personal failure changes the psychological response to it. A person who experiences rising hunger at week eight and interprets it as their body working against them for physiological reasons is more likely to make a rational adjustment than one who interprets the same experience as evidence that they lack the willpower to succeed. The evidence in the cognitive psychology literature supports this framing: psychological reappraisal of challenging experiences reduces their aversive impact without requiring the experience to actually change.
Diet breaks A diet break is a structured period of approximately one to two weeks during which intake is returned to maintenance calories, ending the calorie deficit temporarily before resuming the fat loss phase. Diet breaks allow partial recovery of leptin, partial restoration of glycogen and energy availability, some normalisation of cortisol and mood, and a meaningful recovery of the psychological tolerance required to sustain continued restriction.
Research on diet breaks suggests they can improve long-term fat loss outcomes compared to continuous restriction of the same duration, partly by reducing the degree of adaptive thermogenesis that accumulates, and partly by improving adherence quality when the diet resumes. A diet break is distinct from a period of unstructured eating: the intake target is set deliberately at maintenance rather than simply relaxing dietary restraint.
Refeeds A refeed is a shorter version of the diet break, typically lasting one to two days over a weekend, during which intake is returned to maintenance or a modest surplus primarily through additional carbohydrate. The rationale is that increased carbohydrate intake restores glycogen, temporarily improves training performance and session quality, provides some hormonal benefit through a transient increase in leptin, and gives a psychological respite from the discipline of continuous restriction.
Refeeds are particularly practical for individuals with a defined competition or event timeline who cannot accommodate a full diet break without compromising their schedule. They address the physical and psychological demands of the diet at shorter intervals without meaningfully disrupting the overall progression of the fat loss phase.
When Should a Fat Loss Phase End Entirely?
Diet breaks and refeeds are management tools for extending a productive fat loss phase, but they are not solutions for a phase that has genuinely run its course. Recognising when the appropriate response to diet fatigue is to end the deficit rather than manage around it is a useful coaching skill.
A fat loss phase warrants ending when training performance has declined significantly and is not recovering between sessions despite adequate protein and calorie intake. A diet break completed for the recommended minimum of one to two weeks that does not resolve fatigue signals suggests that the accumulated physiological cost of the diet has exceeded what periodic maintenance eating can address in a short period. When adherence has become effortful enough that the quality of daily life is meaningfully compromised, and when the psychological patterns of restriction and reactivity that are emerging are significant enough to warrant stepping back from an active deficit, continuing into a deeper calorie restriction provides diminishing returns relative to the physiological and psychological cost.
The goal achieved criterion is worth noting separately. Continuing a fat loss phase beyond the point at which the primary goal has been met is a pattern that appears particularly in competitive athletes and physique-focused individuals, where the combination of visible progress and accumulated momentum can make stopping feel counterintuitive. When the goal has been reached, or when the cost of continuing meaningfully exceeds the benefit of further fat loss, returning to maintenance is the appropriate next step.
Understanding when to stop is as strategically important as understanding how to start. A well-timed return to maintenance calories protects training performance, preserves lean mass, allows the hormonal environment to normalise, and puts the individual in a physiological position to benefit from the next structured phase, whether that is a period of muscle building or another fat loss cycle. This decision-making process, including how aggressive the deficit should be, when to implement a break, and when to end the phase entirely, is a central component of how we manage fat loss phases with our coaching clients.
Why Dieting History and Starting Point Affect Diet Fatigue Onset
How quickly and severely diet fatigue sets in varies considerably between individuals, and the factors that drive that variation are largely structural rather than psychological.
Starting body composition is one of the most significant determinants. Individuals with more fat mass to lose at the outset of a diet have a larger energy reserve, which means the same calorie deficit produces a proportionally less severe physiological response than it does in leaner individuals. A person dieting from a higher body fat percentage can sustain a mild deficit for longer before the hormonal and metabolic adaptations described above become clinically significant, because their fat stores are providing a meaningful contribution to the energy deficit alongside dietary restriction.
Leaner individuals, and particularly those who are already carrying a relatively modest body fat, experience the adaptive responses to deficit more acutely and more rapidly. Contest prep athletes pushing through the final weeks of an aggressive cut, well below the body fat levels they would maintain at maintenance, are experiencing diet fatigue in a categorically different context from someone in a moderate deficit with considerably more fat to lose and no external deadline. The same physiological mechanisms are operating, but the deficit is deeper, the fat stores are lower, and the timeline may be non-negotiable.
Dieting history also matters. Individuals who have completed multiple fat loss cycles tend to have a better-calibrated sense of what diet fatigue feels like, which allows them to respond to it earlier and more rationally. First-time dieters, or those who have not previously experienced the later stages of a meaningful deficit, often attribute diet fatigue symptoms to factors other than the diet itself, which delays the appropriate response and allows the fatigue to accumulate further before action is taken.
Practical Takeaways
Diet fatigue is a normal and predictable feature of sustained energy restriction, not a sign of inadequate willpower. The physiological mechanisms behind it, including rising ghrelin, falling leptin, reduced NEAT, adaptive thermogenesis, and declining sleep quality, are well-characterised in the research.
Hunger becomes harder to manage as a diet extends because the hormonal environment shifts in a direction that opposes continued restriction. Recognising this as physiology rather than personal failure is both accurate and practically useful.
Key signals of diet fatigue include declining adherence despite consistent effort, persistent food preoccupation, reduced training performance, irritability, disrupted sleep, and a general fatigue disproportionate to training load. Multiple signals appearing simultaneously is a more meaningful indicator than any single symptom.
Diet breaks of approximately one to two weeks at maintenance calories help restore physical and psychological tolerance for continued dieting and may reduce adaptive thermogenesis accumulation over the long term.
Refeeds of one to two days at maintenance or slight surplus, primarily from carbohydrate, are a practical shorter-term option for individuals with defined timelines who cannot accommodate a full diet break.
Understanding that difficulty is a normal and expected feature of a fat loss phase, established before the diet begins rather than discovered mid-phase, substantially improves the ability to respond to that difficulty rationally.
Knowing when to end a fat loss phase entirely, rather than managing around ongoing fatigue, is as strategically important as knowing how to sustain one.
Frequently Asked Questions
What is diet fatigue and is it the same as a plateau?
Diet fatigue and a weight loss plateau are related but distinct phenomena. A plateau refers specifically to the stalling of scale weight loss despite continued dietary adherence, and is primarily driven by adaptive thermogenesis and NEAT reduction. Diet fatigue is a broader cluster of physiological and psychological symptoms, of which a plateau is one component. Diet fatigue includes declining adherence, disrupted sleep, impaired recovery, reduced training performance, and worsening mood alongside the metabolic adaptations that produce a plateau.
How long does it take for diet fatigue to set in?
The onset of diet fatigue varies considerably based on the severity of the calorie deficit, starting body composition, dieting history, and individual susceptibility. A modest deficit in an individual with significant fat reserves may not produce meaningful fatigue for several months. An aggressive deficit in a leaner individual may produce recognisable symptoms within four to six weeks. Most people in a sustained moderate deficit begin to notice compounding symptoms somewhere between eight and sixteen weeks, which is one reason that periodic diet breaks are recommended for phases longer than ten to twelve weeks.
Does a diet break set back progress?
A well-executed diet break of one to two weeks at maintenance calories does not meaningfully set back fat loss progress over the longer arc of the phase. The scale weight will typically increase slightly as glycogen and water are restored, but this reflects changes in tissue water rather than fat gain. Research on diet breaks suggests they may actually improve long-term outcomes compared to continuous restriction by reducing adaptive thermogenesis accumulation, improving adherence quality on resumption, and partially restoring the hormonal environment that sustained restriction disrupts.
Is it normal to feel irritable and low on a diet?
Yes. Elevated cortisol from prolonged energy restriction, declining leptin, and the psychological demands of continuous dietary regulation all contribute to reduced mood and stress tolerance as a diet extends. This is a recognised feature of sustained calorie restriction and not a reflection of psychological weakness or an indicator that the diet approach is wrong. It typically resolves when intake is returned to maintenance and becomes a signal for intervention when it is severe enough to meaningfully affect daily function or relationships.
What is adaptive thermogenesis and how does it affect fat loss?
Adaptive thermogenesis refers to the reduction in total daily energy expenditure that occurs during sustained energy restriction beyond what would be predicted from mass loss alone. As the body detects a prolonged calorie deficit, it reduces metabolic rate through multiple mechanisms including reductions in thyroid hormone activity, sympathetic nervous system output, and spontaneous physical activity. The practical effect is that the same calorie intake produces progressively less fat loss over time, and a diet break or the end of the phase may be needed before the next productive deficit can be applied.
Should training intensity change during a fat loss phase to manage diet fatigue?
Training volume and intensity should ideally be maintained as close to the normal baseline as the diet allows, because maintaining training performance is one of the most effective strategies for preserving lean mass during a deficit. A sustained and significant decline in performance that is not recovering between sessions is a signal that the deficit is too aggressive rather than a prompt to train less. The appropriate response in most cases is to adjust the calorie deficit rather than substantially reduce training demand. Monitoring training performance using RPE or reps in reserve provides a sensitive early indicator of when dietary adjustments are warranted.
Managing diet fatigue well, from calibrating the deficit appropriately to knowing when to implement a break or end the phase entirely, requires a level of individual adjustment that is difficult to apply without ongoing feedback. If you want support navigating a fat loss phase with that level of precision, you can enquire about coaching or book a consultation to get started.